Physiotherapy After Joint Replacement: What To Expect
- SMARTPHYSIO
- Mar 1
- 3 min read
Updated: Apr 21
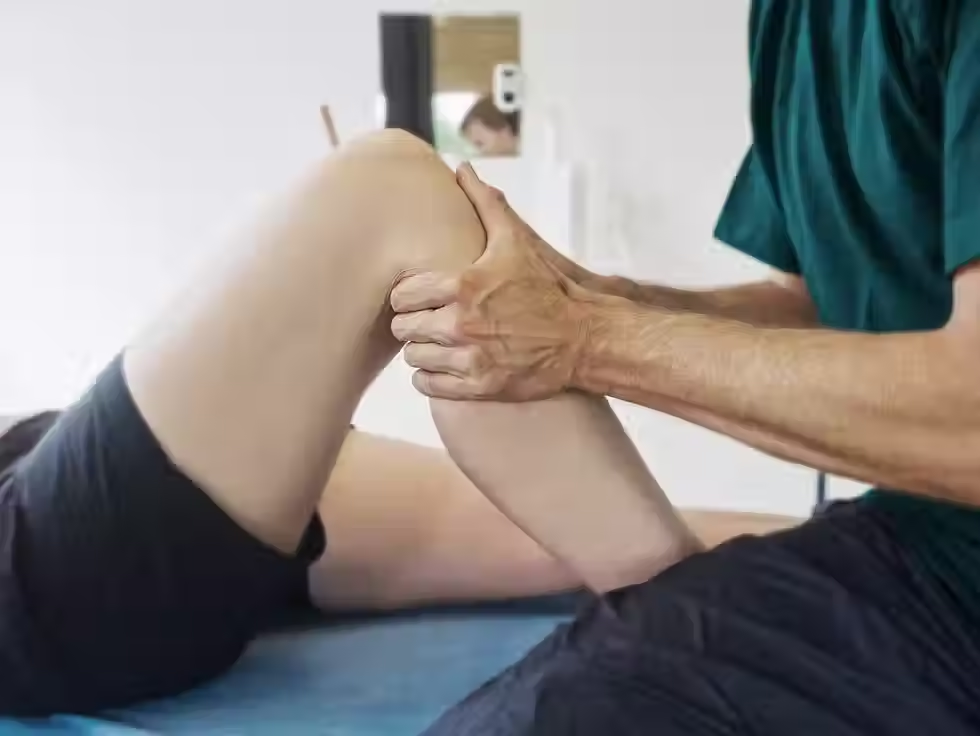
Joint replacement surgery is a major step toward regaining comfort and mobility, but it is only the beginning of the recovery process. Physiotherapy plays a central role in helping patients rebuild strength, improve function, and return to everyday activities with confidence. While every recovery journey is unique, understanding the general stages can make the experience feel more predictable and manageable.
Below is a guide that outlines what many patients can expect after a hip or knee replacement. It is designed to offer reassurance, highlight the value of consistent rehabilitation, and explain how physiotherapists support progress at each stage.
Stage 1: Early Mobility and Pain Control
During the first stage, the focus is on gentle movement and establishing a safe routine. Most patients begin standing and taking short steps with assistance on the day of or the day after surgery. A physiotherapist will guide these early movements, provide advice on how to get in and out of bed safely, and teach exercises that help prevent stiffness.
Swelling and discomfort are normal at this stage, so rest, ice, and appropriate medication are important. Simple circulation exercises, such as ankle pumps and gentle bending and straightening of the knee or hip, begin early to reduce the risk of complications and encourage blood flow.
Stage 2: Building Confidence With Basic Activities
By the second week, many patients are beginning to feel more confident with short walks inside the home. Physiotherapists often introduce slightly more challenging exercises, focusing on improving the range of movement and activating weakened muscles. The goal isn’t to push through pain, but to practise steady, consistent activity.
Reinforcing good walking technique is essential. Even small details, like foot placement and upright posture, make a noticeable difference in how efficiently someone moves and how quickly they progress.
Stage 3: Increasing Strength and Reducing Assistance
As the early healing period settles, exercises typically expand to include more purposeful strength and balance work. Patients often begin walking longer distances and may start using a single crutch or walking stick instead of two. Physiotherapists monitor how the joint is responding and adjust the plan to match individual progress.
Activities such as climbing stairs, standing from a chair without using the arms, and gentle balance exercises help people regain independence. Many patients feel their confidence growing at this stage, though it is still important to avoid rushing or overloading the joint.
Stage 4: Returning to Everyday Routines
Around one month after surgery, patients usually begin to notice meaningful improvements. Daily tasks feel easier, walking becomes more natural, and strength begins to return. Physiotherapists often introduce exercises that challenge the joint in more functional positions, as well as guidance for gradually returning to hobbies or light household activities.
For those who enjoyed regular exercise before surgery, this period is often the point where low impact options, such as cycling on a stationary bike or swimming (once the wound has healed), may be introduced. The aim is to rebuild stamina without placing unnecessary stress on the new joint.
Stage 5: Building Long-Term Strength and Mobility
During this stage, physiotherapy focuses on long-term recovery. The joint is settling, coordination is improving, and most patients are able to walk more freely. Strength and control around the hip or knee are key areas of focus, as these muscles provide the joint with the support it needs for daily movement.
Physiotherapists may progress exercises to include more dynamic activities, such as step-ups, balance challenges, or resistance work. Each programme is tailored to match individual ability and goals, whether that is returning to gardening, longer walks, or more advanced exercise.
Ongoing Physio Progress
Although many people feel settled by the three-month mark, full recovery continues for much longer. Strength, endurance, and confidence can keep improving with guided physiotherapy. Regular review sessions help identify small issues before they develop and provide reassurance about what level of activity is safe.
The most successful recoveries come from steady, consistent progress rather than speed. Patience, guidance, and exercise all work together to help the new joint feel as natural and reliable as possible.
How We Can Help After Joint Replacement Surgery
At SmartPhysio, we support people recovering from hip and knee replacement surgery with tailored rehabilitation focused on strength, mobility and confidence. Whether you are just home from hospital or looking to improve longer-term recovery, our experienced team can help you progress safely. Explore Pre&post Surgery, Home Visits, Physiotherapy, or contact us to arrange an assessment.



